Author: Nihal M. El Rouby, PharmD, PhD on November 01, 2023 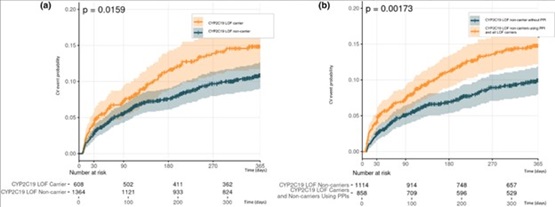
Clopidogrel, a widely prescribed antiplatelet medication, varies in its effectiveness due to multiple factors, including genetics and drug interactions. The CYP2C19 enzyme plays a key role in converting clopidogrel into its active form. Individuals carrying CYP2C19 loss-of-function (LOF) alleles have reduced ability to convert clopidogrel to its active metabolite. Hence, these patients are at an increased risk of higher on-clopidogrel, platelet reactivity, recurrent thrombo-embolic events and major cardiovascular events (MACE), compared to patients without LOF alleles. Proton pump inhibitors (PPIs) are often co-prescribed with clopidogrel for gastric protection and can competitively inhibit the CYP2C19, resulting in a phenomenon called "phenoconversion" – and potentially leading to an elevated risk of MACE. The extent of CYP2C19 inhibition varies among PPIs, with omeprazole and esomeprazole documented to be the most potent inhibitors. However, studies evaluating the impact of PPIs on clopidogrel effectiveness have generated conflicting results. Some data show no significant impact of PPIs on MACE, and others show increased risk of cardiovascular events, and only a few studies have simultaneously assessed both CYP2C19 and PPI use.
To address this knowledge gap, a study conducted by Markus Ramste, Markus Ritvos, and Sergei Häyrynen et al., and published in Clinical and Translational Science, assessed the impact of CYP2C19 and PPI-induced phenoconversion of CYP2C19 in patients with acute coronary syndrome (ACS) or stable symptomatic chronic coronary disease. This real-world data/real-world evidence (RWD/RWE) study included 1,972 patients on clopidogrel from Corogene, a Finnish registry, with clopidogrel use confirmed via the Finnish prescription registry. The patients were followed for 365 days and evaluated for MACE, including myocardial infarction, ischemic stroke, and cardiovascular death. During the follow-up period, carriers of CYP2C19 LOF alleles experienced a higher incidence of new cardiovascular events (14.8%, 95% CI, 11.7–17.8), compared to non-carriers (10.8%, 95% CI, 9.0–12.6), (Figure A). Interestingly, among patients who were using PPIs, the non-carriers of CYP2C19 LOF alleles who were using PPIs and the LOF carriers were at a significantly higher risk of MACE compared to LOF non-carriers who were not using these PPIs (Figure B).
These RWD show the interplay between CYP2C19 and drug interaction in predicting the effectiveness of clopidogrel and highlight the importance of considering patients' factors, including phenoconversion, when prescribing P2Y12 inhibitors.

The comment feature is locked by administrator.